About Us
Canadians see a primary care provider at multiple points in life: from well-baby visits to end-of-life planning. A primary care provider could be a family physician, nurse practitioner, or other trained health professional and are generally the first called when people have a health concern.
Research has shown the strongest clinical evidence for improving health outcomes in the population is by strengthening primary care. When people have access to strong primary care, they can address a health concern before it leads to a trip to the hospital. So, not only does primary care keep people healthy, it saves health care dollars.
The David Braley Primary Care Research Collaborative (PCRC) was launched in September 2020 to further advance research to strengthen primary care systems through a $4 million investment — seeded by a $1 million contribution by David Braley. This collaborative is the first of its kind in Canada, with the largest endowment supporting a research collaborative in primary care.
The PCRC is bringing together researchers, clinicians, educators and partners to work on issues that will address the diverse needs of our community. We are focused on:
- Building research capacity throughout primary care
- Developing networks of experts, mentors and trainees
- Contributing new evidence to the field of primary care research
- Sharing and implementing knowledge when and where it is needed
- Influencing policy change to improve the health of our communities
Information Box Group
We’re building capacity Research Supports
Resources for growing your primary care research practice.
We’re leading change Research Programs
Learn more about a few of the ways our collaborative is changing primary care.
We’re creating a network of experts Our Researchers
Learn about some of the experts in our network and their research.
Our Research
Researchers, clinicians and staff in the department are engaged in practice-based research focused on building innovative systems of primary care using mixed methods, qualitative, and quantitative research designs. The team is working on initiatives to enhance the care that people receive, to improve access to health care particularly for people in greatest need and to change the way the next generation of clinicians are trained.
Information Box Group

We embrace a culture of evidence-informed primary care by working to discover new knowledge and creating new ways to improve the health care patients receive — so that they may enjoy a life worth living on their terms.
Our research, which has informed the development of innovative systems of care and contributed knowledge leading to improved health outcomes, is regularly recognized with local, provincial, national and international awards for excellence.
Information Box Group
$40 million dollars of research funding in the past ten years
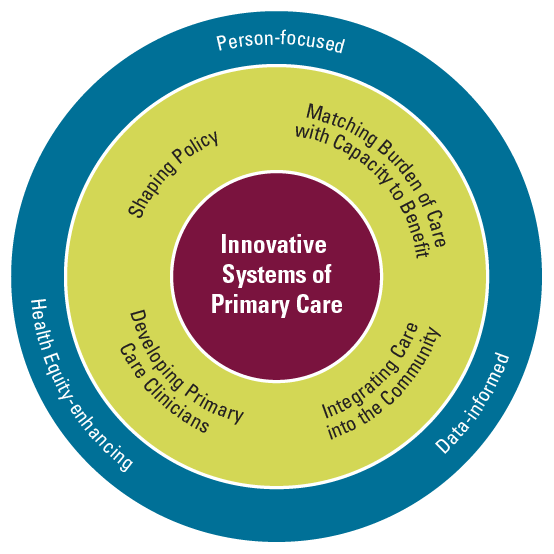
Research clusters
Shaping Policy
Policies are an influential element shaping health care delivery. We aim to shape policy through our research and consider the ethical and social implications of health policies to ensure the delivery of sensitive and responsive care.
Developing Primary Care Clinicians
The education and development of clinician trainees is an important part of DFM work and several faculty members are involved in researching how to do this more effectively. Research considers the development of the practicing primary care clinician, drawing attention to how they navigate difficult circumstances, enhance their skillset, and keep up to date.
Integrating Care into the Community across the Lifespan
We have a focus with delivering care to patients where they need it most, which is often in the community. This might mean meeting patients where they are, whether this is elderly people at home, in subsidised housing or in places of incarceration.
Matching Burden of Care with Capacity to Benefit
Established health system practices may not be the best use of resources for patients or for the system. Many of our researchers are considering scenarios that see a potentially high burden of care for a relatively low treatment benefit e.g., overdiagnosis, multimorbidity.
Cross-cutting values
Person-focused
Patient, family, and primary care clinician are the ‘person’ at the centre of the work we do, with particular attention to patient priorities and preferences in clinical care.
Data-informed
Data is important in describing, understanding and shaping practice patterns, the training of clinicians, and identifying places for improving efficiency, efficacy or safety of care.
Health equity-enhancing
Our researchers work to understand and alleviate health inequities experienced by many different types of equity-seeking groups, including racialized and Indigenous populations, gender-diverse and queer populations.
Research News
Information Box Group

McMaster researchers map maternal and infant health in Morocco with new scoping review
News, Research
July 18, 2024

McMaster Graduate Studies ➚
Monika Dutt receives 2024 Vanier Canada Graduate Scholarship as PhD candidate under supervision of Meredith Vanstone
News, Research
June 24, 2024

Developing a physician continuity of care index for end-of-life care
Primary Care Late Life, Research Project Update
May 30, 2024

COVID-19 Pandemic impacted the frequency of key primary care activities according to national study
News, Research, RIPPLE-C
May 22, 2024
Research Supports and Funding
Research at the Department of Family Medicine is a broad (and growing) area of focus. To help research projects initiate, expand and share knowledge, we provide a number of resources that have been designed to help our faculty, our staff and the broader primary care research community.
Information Box Group

Pilot Research Project Funding Learn More
The departments funds pilot projects (maximum $5,000 each) for faculty members to conduct research in primary care, palliative care and medical education.

Research Knowledge and Skill Builder Sessions Learn More
We offer monthly in-services to continue to build the research capacity of faculty and staff across the department.

TRAction: A Toolkit for Research in Action Learn More
A curated collection of resources mapped to the steps of the research process from project design to implementation and knowledge translation.

Research Group Learn More
People are at the heart of our research. We have made strategic investments to build a highly skilled staffing infrastructure to support and promote innovative primary care research involving over 15 distinct research teams.

Research Advice Café
Senior researchers offer mentorship to faculty members who are less experienced in research, providing advice and support to develop their research idea. Email pcrc@mcmaster.ca to connect.

Primary Care Research: A Pathway for Learning
This open-access online course guides learners through four steps to enhance their primary care research skills using a curated selection of tools from TRAction: A Toolkit for Research in Action. Learners can complete all four steps or select the modules that meet their specific learning needs. Please email pcrc@mcmaster.ca to access the course.

Health Sciences Library Learn More
Additional research supports are available through the Health Sciences Library for access to books, journals and e-resources and consultations with a librarian for literature search and review.
Research Leadership and Support
Our research group leadership consists of a Research Director, administrators and knowledgeable staff who support efficient, effective and high-quality research projects.
Fiona Kouyoumdjian
MD, MPH, PhD, FCFP, FRCPC
Assistant Professor
Research Director
ResearchGate
David Braley Health Sciences Centre
@F_Kouyoumdjian
fiona-kouyoumdjian-b4a2a920
McMaster Experts Profile
Fiona Kouyoumdjian is a Family Physician, Public Health and Preventive Medicine Physician, and Epidemiologist. She received her BA with Honors from Brown University, her MD from Dalhousie University, her MPH from the Johns Hopkins Bloomberg School of Public Health, and her PhD in Epidemiology from the University of Toronto Dalla Lana School of Public Health. She completed residency training at the University of Toronto and a CIHR Fellowship at St. Michael’s Hospital.
Fiona leads a program of research focused on the health status and health care of people who experience imprisonment. Her specific research foci are decreasing imprisonment, improving health care and health promotion for people in prison, and supporting successful re-integration to the community for people on release from prison.
Fiona is also an Adjunct Scientist at ICES and an Associate Member in the Department of Health Research Methods, Evidence, and Impact at McMaster.

Fiona Kouyoumdjian
MD, MPH, PhD, FCFP, FRCPC
Assistant Professor
Research Director
Laura Cleghorn
Manager, Research
Laura Cleghorn has conducted research about the organization and delivery of health care in Ontario for over 15 years in the areas of home care, primary care, and cancer care, often focused on improving access to care for marginalized populations. Since 2016, Laura has been with the Department of Family Medicine in a role that supports the faculty and staff of the Research Enterprise to engage in high-quality research. Laura is also interested in cultivating a workplace culture that encourages personal and professional growth. When not at work, Laura can be found in arenas in the greater Hamilton area, enjoying her kids’ hockey and figure skating activities. Laura’s second favourite past-time is walking her dog in Cootes Paradise, in all seasons.
Bethany Elliott
BHSc, MPH
Administrative Director, David Braley Primary Care Research Collaborative
Bethany is the Administrative Director of the David Braley Primary Care Research Collaborative (PCRC). In this role, she supports the development and expansion of a network to explore important questions in primary care and amplify evidence to inform primary care practice, education, and health systems planning. Bethany has a Master of Public Health in health promotion and community development and prior to joining the PCRC worked in the public health sector in British Columbia and Ontario for over a decade. Through this work, Bethany collaborated regularly with health system partners, local and provincial governments and community organizations on projects ranging from health promotion and evaluation to health systems planning. Most recently, she provided strategic and operational support to the Hamilton COVID-19 Response Table – a collaborative table chaired by public health, primary care, and hospitals to prevent and respond to COVID-19 in Hamilton.

Bethany Elliott
BHSc, MPH
Administrative Director, David Braley Primary Care Research Collaborative
Erin Beaulieu
RD, MPH
Manager, Knowledge Translation and Strategic Communications
Erin Beaulieu has worked for the Department of Family Medicine since March 2019 as a Knowledge Translation (KT) Specialist and then moved into the role of KT and Strategic Communications Manager in February 2022. In this role, she provides leadership, guidance and support for targeted, responsive and effective KT and communications initiatives across all departmental domains to further strategic objectives, strengthen internal and external engagement, enable greater research impact by furthering the uptake of evidence into practice and policy. Prior to joining McMaster University, Erin worked as a Registered Dietitian in public health and supporting local food policy and programs in the provincial government. Erin holds a Bachelor of Applied Science in Applied Human Nutrition and a Masters of Public Health in Community Nutrition. When she’s not at work, Erin enjoys cooking, cycling, and cuddling with her cat, Ollie.

Erin Beaulieu
RD, MPH (on leave)
Manager, Knowledge Translation and Strategic Communications
Information Box Group
Neha Arora
Clinic Research Coordinator
Neha has been a part of McMaster since 2011 working in DFM since 2014 on the iGAP study. She is a trained physiotherapist and her research interests are in the care of the elderly.
Brittney Bowen
Administrative Assistant
Patricia Habran-Dietrich
BA
Administrative Assistant (on LOA)
Patricia Habran-Dietrich joined McMaster in 2013, as an administrative assistant for the Aging, Community and Health Research Unit (ACHRU), within the School of Nursing. In mid- 2014, Patricia joined the Department of Family Medicine as part of the HOPE program. Since 2015 she has been a member of the Research Enterprise, providing direct support to Drs. Dee Mangin and Michelle Howard in their research administrative tasks, as well as broadly supporting the staff of the research team.
Her broad interests include travel, reading and meeting people from diverse backgrounds.

Patricia Habran-Dietrich
BA
Administrative Assistant (on LOA)
Casey Irvin
MA
Manager, Knowledge Translation and Strategic Communications
Casey Irvin works to amplify our department’s impact.
As the manager of knowledge translation and strategic communications at the department of family medicine (DFM), he supports faculty, staff and learners to help connect their ideas, research and purpose to key audiences.
Casey worked with DFM for six years as both a communications coordinator and as the department’s first knowledge translation specialist before joining the McMaster Institute for Research on Aging in 2021. Returning to DFM in 2024 (to cover a leave for Erin Beaulieu), Casey is a steadfast advocate for creating progressive, equitable improvements to health care through effective communication, knowledge mobilization and telling good stories.
He has a master’s degree in communications and cultural studies and over 15 years of communications experience in the health care, education and social services sectors.
Advina Kamaric
MPH
Knowledge Translation Specialist
Advina Kamaric has been working for the Department of Family Medicine since July 2023. In her role as Knowledge Translation Specialist, she works with DFM researchers to raise awareness of the outcomes of research projects in the department through the development of various knowledge translation products such as infographics, videos, reports, and social media posts.
Advina holds a Bachelor of Science in Health Studies with a Specialization in Health Research and a Master of Public Health.
Outside of work, Advina enjoys traveling, baking, and reading.
Jennifer Lawson
Business Analyst
Jennifer has been a McMaster employee since 2002 and came to join the DFM in the fall of 2015, as part of the MUSIC (McMaster University Sentinel Information and Collaboration) team operating as a Primary Care Research Network. She has a background in Information Science and has applied that to Evidence-based Medicine literature delivery projects and services. More recent training in Health Informatics has had her interest peaked in leveraging primary care data to answer questions about how best to deliver quality care. Toward this work she is currently surveying the data collected in OSCAR for its fit of use and strategizing toward better data capture and data quality improvement initiatives. Jennifer lives in Dundas, Ontario with her husband and daughter and newly rescued dog.
Special Interests
Gardening
Outdoor Recreation (hiking
canoeing
biking)
Canadian music
Jennifer Salerno
MSc, PhD
Research Associate
Dr. Jennifer Salerno’s research interests include chronic disease epidemiology and the application of epidemiology methods to trial research, population and public health, and health services research. She holds a PhD in Epidemiology from the University of Toronto, MSc in Community Health and Epidemiology from Queen’s University, and Honours BSc from McMaster University’s Biology and Pharmacology Co-operative Program. She completed fellowship training at both the Toronto Rehabilitation Institute in the area of traumatic brain injury epidemiology and the U.S. National Institutes of Health (National Cancer Institute’s Hormonal and Reproductive Epidemiology Branch) in the area of breast cancer epidemiology. Her previous research interests included studying the epidemiology of brain injuries and related vascular dementias, and specifically, examining the etiology of cognitive function in aging populations using molecular/biochemical methods and advanced statistical models. She previously worked for several years as a clinical epidemiologist in the Government of Ontario (MOHLTC and Health Quality Ontario) where she performed several health technology assessments, systematic reviews and meta-analyses. She also developed cancer clinical practice guidelines supporting Cancer Care Ontario’s Cancer Imaging Program through McMaster’s Program in Evidence-Based Care, Department of Oncology.
Currently, at McMaster University, she is a Research Associate for the Department of Family Medicine. She is involved in the TAPER research study (TAPER: Team Approach to Polypharmacy Evaluation and Reduction) which aims to reduce multiple medication use and the harmful effects of polypharmacy among older adults. She is also involved with the Primary Care Research Collaborative (PCRC) in the Department of Family Medicine by providing clinical faculty teaching and mentoring initiatives and opportunities and developing the patient/public/community advisory group for the PCRC. She currently teaches in the health research methodology program in the Department of Health Research Methods, Evidence, and Impact at McMaster and is currently the Vice Chair of the American College of Epidemiology (ACE) Ethics Committee. She has held numerous leadership positions in ACE and more recently, she is involved with the International Epidemiological Association as the North American Regional Councillor.
Michelle Sylvain
Administrative Coordinator
Michelle joined McMaster’s Department of Family Medicine in August 2019 as the Research Administrative Coordinator. She transitioned to administrative work in 2015 after 10 years in broadcasting. Michelle enjoys cooking in her spare time and travelling whenever possible.
Neha Arora
Clinic Research Coordinator
Neha has been a part of McMaster since 2011 working in DFM since 2014 on the iGAP study. She is a trained physiotherapist and her research interests are in the care of the elderly.
Neha Arora
Clinic Research Coordinator
Neha has been a part of McMaster since 2011 working in DFM since 2014 on the iGAP study. She is a trained physiotherapist and her research interests are in the care of the elderly.
Brittney Bowen
Administrative Assistant
Brittney Bowen
Administrative Assistant
Patricia Habran-Dietrich
BA
Administrative Assistant (on LOA)
Patricia Habran-Dietrich joined McMaster in 2013, as an administrative assistant for the Aging, Community and Health Research Unit (ACHRU), within the School of Nursing. In mid- 2014, Patricia joined the Department of Family Medicine as part of the HOPE program. Since 2015 she has been a member of the Research Enterprise, providing direct support to Drs. Dee Mangin and Michelle Howard in their research administrative tasks, as well as broadly supporting the staff of the research team.
Her broad interests include travel, reading and meeting people from diverse backgrounds.
Patricia Habran-Dietrich
BA
Administrative Assistant (on LOA)
Patricia Habran-Dietrich joined McMaster in 2013, as an administrative assistant for the Aging, Community and Health Research Unit (ACHRU), within the School of Nursing. In mid- 2014, Patricia joined the Department of Family Medicine as part of the HOPE program. Since 2015 she has been a member of the Research Enterprise, providing direct support to Drs. Dee Mangin and Michelle Howard in their research administrative tasks, as well as broadly supporting the staff of the research team.
Her broad interests include travel, reading and meeting people from diverse backgrounds.
Casey Irvin
MA
Manager, Knowledge Translation and Strategic Communications
Casey Irvin works to amplify our department’s impact.
As the manager of knowledge translation and strategic communications at the department of family medicine (DFM), he supports faculty, staff and learners to help connect their ideas, research and purpose to key audiences.
Casey worked with DFM for six years as both a communications coordinator and as the department’s first knowledge translation specialist before joining the McMaster Institute for Research on Aging in 2021. Returning to DFM in 2024 (to cover a leave for Erin Beaulieu), Casey is a steadfast advocate for creating progressive, equitable improvements to health care through effective communication, knowledge mobilization and telling good stories.
He has a master’s degree in communications and cultural studies and over 15 years of communications experience in the health care, education and social services sectors.
Casey Irvin
MA
Manager, Knowledge Translation and Strategic Communications
Casey Irvin works to amplify our department’s impact.
As the manager of knowledge translation and strategic communications at the department of family medicine (DFM), he supports faculty, staff and learners to help connect their ideas, research and purpose to key audiences.
Casey worked with DFM for six years as both a communications coordinator and as the department’s first knowledge translation specialist before joining the McMaster Institute for Research on Aging in 2021. Returning to DFM in 2024 (to cover a leave for Erin Beaulieu), Casey is a steadfast advocate for creating progressive, equitable improvements to health care through effective communication, knowledge mobilization and telling good stories.
He has a master’s degree in communications and cultural studies and over 15 years of communications experience in the health care, education and social services sectors.
Advina Kamaric
MPH
Knowledge Translation Specialist
Advina Kamaric has been working for the Department of Family Medicine since July 2023. In her role as Knowledge Translation Specialist, she works with DFM researchers to raise awareness of the outcomes of research projects in the department through the development of various knowledge translation products such as infographics, videos, reports, and social media posts.
Advina holds a Bachelor of Science in Health Studies with a Specialization in Health Research and a Master of Public Health.
Outside of work, Advina enjoys traveling, baking, and reading.
Advina Kamaric
MPH
Knowledge Translation Specialist
Advina Kamaric has been working for the Department of Family Medicine since July 2023. In her role as Knowledge Translation Specialist, she works with DFM researchers to raise awareness of the outcomes of research projects in the department through the development of various knowledge translation products such as infographics, videos, reports, and social media posts.
Advina holds a Bachelor of Science in Health Studies with a Specialization in Health Research and a Master of Public Health.
Outside of work, Advina enjoys traveling, baking, and reading.
Jennifer Lawson
Business Analyst
Jennifer has been a McMaster employee since 2002 and came to join the DFM in the fall of 2015, as part of the MUSIC (McMaster University Sentinel Information and Collaboration) team operating as a Primary Care Research Network. She has a background in Information Science and has applied that to Evidence-based Medicine literature delivery projects and services. More recent training in Health Informatics has had her interest peaked in leveraging primary care data to answer questions about how best to deliver quality care. Toward this work she is currently surveying the data collected in OSCAR for its fit of use and strategizing toward better data capture and data quality improvement initiatives. Jennifer lives in Dundas, Ontario with her husband and daughter and newly rescued dog.
Special Interests
Gardening
Outdoor Recreation (hiking
canoeing
biking)
Canadian music
Jennifer Lawson
Business Analyst
Jennifer has been a McMaster employee since 2002 and came to join the DFM in the fall of 2015, as part of the MUSIC (McMaster University Sentinel Information and Collaboration) team operating as a Primary Care Research Network. She has a background in Information Science and has applied that to Evidence-based Medicine literature delivery projects and services. More recent training in Health Informatics has had her interest peaked in leveraging primary care data to answer questions about how best to deliver quality care. Toward this work she is currently surveying the data collected in OSCAR for its fit of use and strategizing toward better data capture and data quality improvement initiatives. Jennifer lives in Dundas, Ontario with her husband and daughter and newly rescued dog.
Special Interests
Gardening
Outdoor Recreation (hiking
canoeing
biking)
Canadian music
Jennifer Salerno
MSc, PhD
Research Associate
Dr. Jennifer Salerno’s research interests include chronic disease epidemiology and the application of epidemiology methods to trial research, population and public health, and health services research. She holds a PhD in Epidemiology from the University of Toronto, MSc in Community Health and Epidemiology from Queen’s University, and Honours BSc from McMaster University’s Biology and Pharmacology Co-operative Program. She completed fellowship training at both the Toronto Rehabilitation Institute in the area of traumatic brain injury epidemiology and the U.S. National Institutes of Health (National Cancer Institute’s Hormonal and Reproductive Epidemiology Branch) in the area of breast cancer epidemiology. Her previous research interests included studying the epidemiology of brain injuries and related vascular dementias, and specifically, examining the etiology of cognitive function in aging populations using molecular/biochemical methods and advanced statistical models. She previously worked for several years as a clinical epidemiologist in the Government of Ontario (MOHLTC and Health Quality Ontario) where she performed several health technology assessments, systematic reviews and meta-analyses. She also developed cancer clinical practice guidelines supporting Cancer Care Ontario’s Cancer Imaging Program through McMaster’s Program in Evidence-Based Care, Department of Oncology.
Currently, at McMaster University, she is a Research Associate for the Department of Family Medicine. She is involved in the TAPER research study (TAPER: Team Approach to Polypharmacy Evaluation and Reduction) which aims to reduce multiple medication use and the harmful effects of polypharmacy among older adults. She is also involved with the Primary Care Research Collaborative (PCRC) in the Department of Family Medicine by providing clinical faculty teaching and mentoring initiatives and opportunities and developing the patient/public/community advisory group for the PCRC. She currently teaches in the health research methodology program in the Department of Health Research Methods, Evidence, and Impact at McMaster and is currently the Vice Chair of the American College of Epidemiology (ACE) Ethics Committee. She has held numerous leadership positions in ACE and more recently, she is involved with the International Epidemiological Association as the North American Regional Councillor.
Jennifer Salerno
MSc, PhD
Research Associate
Dr. Jennifer Salerno’s research interests include chronic disease epidemiology and the application of epidemiology methods to trial research, population and public health, and health services research. She holds a PhD in Epidemiology from the University of Toronto, MSc in Community Health and Epidemiology from Queen’s University, and Honours BSc from McMaster University’s Biology and Pharmacology Co-operative Program. She completed fellowship training at both the Toronto Rehabilitation Institute in the area of traumatic brain injury epidemiology and the U.S. National Institutes of Health (National Cancer Institute’s Hormonal and Reproductive Epidemiology Branch) in the area of breast cancer epidemiology. Her previous research interests included studying the epidemiology of brain injuries and related vascular dementias, and specifically, examining the etiology of cognitive function in aging populations using molecular/biochemical methods and advanced statistical models. She previously worked for several years as a clinical epidemiologist in the Government of Ontario (MOHLTC and Health Quality Ontario) where she performed several health technology assessments, systematic reviews and meta-analyses. She also developed cancer clinical practice guidelines supporting Cancer Care Ontario’s Cancer Imaging Program through McMaster’s Program in Evidence-Based Care, Department of Oncology.
Currently, at McMaster University, she is a Research Associate for the Department of Family Medicine. She is involved in the TAPER research study (TAPER: Team Approach to Polypharmacy Evaluation and Reduction) which aims to reduce multiple medication use and the harmful effects of polypharmacy among older adults. She is also involved with the Primary Care Research Collaborative (PCRC) in the Department of Family Medicine by providing clinical faculty teaching and mentoring initiatives and opportunities and developing the patient/public/community advisory group for the PCRC. She currently teaches in the health research methodology program in the Department of Health Research Methods, Evidence, and Impact at McMaster and is currently the Vice Chair of the American College of Epidemiology (ACE) Ethics Committee. She has held numerous leadership positions in ACE and more recently, she is involved with the International Epidemiological Association as the North American Regional Councillor.
Michelle Sylvain
Administrative Coordinator
Michelle joined McMaster’s Department of Family Medicine in August 2019 as the Research Administrative Coordinator. She transitioned to administrative work in 2015 after 10 years in broadcasting. Michelle enjoys cooking in her spare time and travelling whenever possible.
Michelle Sylvain
Administrative Coordinator
Michelle joined McMaster’s Department of Family Medicine in August 2019 as the Research Administrative Coordinator. She transitioned to administrative work in 2015 after 10 years in broadcasting. Michelle enjoys cooking in her spare time and travelling whenever possible.













